Fears about a boom in COVID positive cases since the easing of restrictions may have lessened across NSW, however, north of Sydney it's a different story.
Subscribe now for unlimited access.
$0/
(min cost $0)
or signup to continue reading
The Mid Coast local government area (LGA), an area from Tea Gardens in the south to Taree to the north, and west to Gloucester, has seen a rise in cases and until only recently topped the list of number of cases per LGA in the Hunter New England Local Health District (HNELHD) which includes the cities of Newcastle and Maitland.
The Mid Coast region did not have a case in the latest outbreak until one week before lockdown ended when a COVID positive person from Sydney came to the area and the virus infiltrated the Aboriginal community. Cases in the Mid Coast steadily spread and peaked at 18 new cases a day, with schools across the region continuously shutting due to positive cases.
However, vaccination rates are higher in the Mid Coast than the State average, and even better in the Mid North Coast Health District which encompasses a region from Port Macquarie to Coffs Harbour.
Read more:
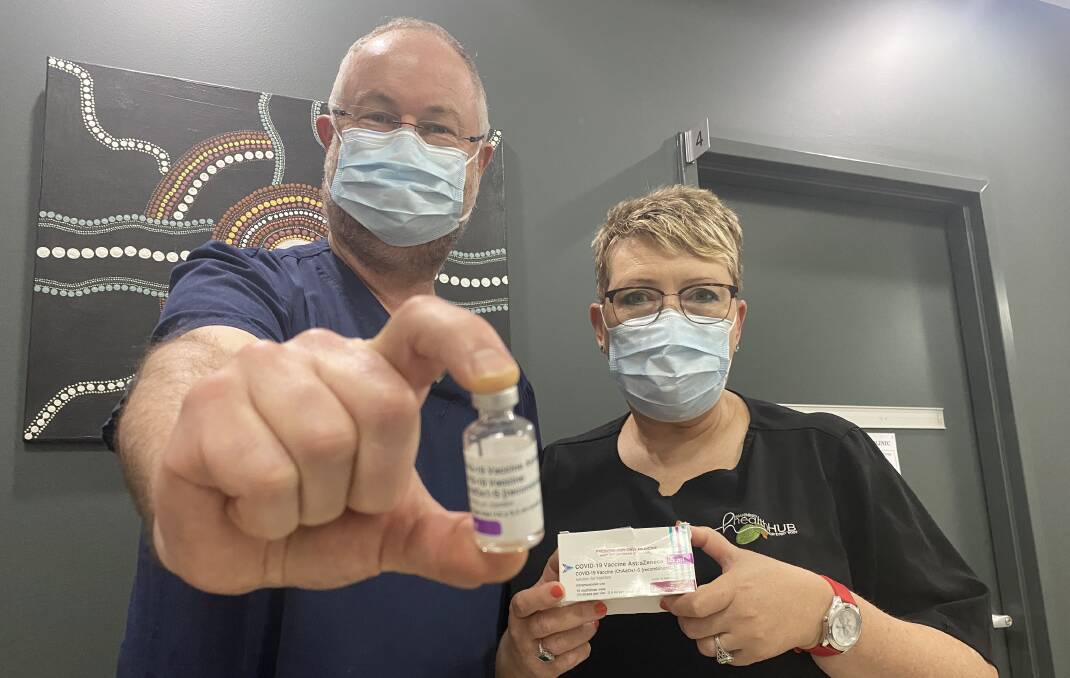
Dr Simon Holliday, a general practitioner on the Mid North Coast who also runs the Commonwealth-supported Taree Respiratory Clinic which delivers COVID-19 vaccination and testing, is very pleased with the high vaccination rates across the region.
"I think it's terrific. I think a lot of people have been so frightened about COVID. They've been angry that they can't have their life the way they want it. They have this incredible pain at the loss of the things they hold dear in their life - relationships, activities - it's been a really difficult time for people," Dr Holliday said.
"The problem is things might seem to be going alright but then they can go pear shaped very, very fast.
"I guess with small hospitals what will happen is that people will do their very best, but we don't have the capacity."
Paramedics and nursing staff in rural and regional areas keep saying there is a chronic staff shortage, and that the capacity of a hospital to deal with an increase in COVID cases will not come down to a lack of beds, but a lack of staff.
Tim McEwan, an Australian Paramedics Association delegate and working paramedic from Yamba, near Coffs Harbour, says that staff are "dead on their feet"
"It's been relentless. Not necessarily COVID related, just generally speaking," Mr McEwen said.
"What we're finding now is that both NSW Ambulance and the hospitals are struggling to staff their units. Even NSW Ambulance can be two or three cars short each shift, and they just can't find paramedics to fill them. The casuals don't seem to be putting their hand up as much; certainly the full time staff are not putting their hands up for overtime.
It's been relentless. Not necessarily COVID related, just generally speaking.
- Tim McEwen, Australian Paramedics Association delegate and Yamba paramedic
"If the hospitals can't staff their wards, then the flow on is that the ED can't get their patients out of there onto the wards," Tim says.
It's a concern repeated by Mark Brennan, president of the NSW Nurses and Midwives Association Port Macquarie Base Hospital branch.
Mark says Port Macquarie Base Hospital is currently 94.41 full time equivalent positions down.
"For a rural hospital like Port Macquarie to have 95 FTE vacancies, It's shameful," Mark said.
"As you can imagine, to pick up those hours that are short, they're relying on nursing staff to do overtime. They are also relying on agency nurses."
When asked about staffing levels at Port Macquarie Base Hospital, Stewart Dowrick, chief executive Mid North Coast Local Health District said that in the last financial year the hospital has increased its nursing numbers by 44 full time staff.
The resilience of the staff - the paramedics and hospital staff - is wearing pretty thin.
- Tim McEwen
"While there are a number of vacancies, we continue to actively recruit to these positions," Mr Dowrick said.
"Some of these temporary vacancies are the result of permanent staff taking up opportunities to assist the District's COVID-19 response in areas such as testing, vaccination and caring for COVID-positive patients and their families in the community."
The onus on existing health workers has Tim McEwen concerned for the future, despite his region not fighting on the battle front of COVID-19.
"I worry about resilience of the health system to be able to deal with anything that does come up, which was much like it was before and seeing the struggles that we're having, probably more so," Mr McEwen said.
"The resilience of the staff - the paramedics and hospital staff - is wearing pretty thin. We're already pretty dead on our feet."
Our journalists work hard to provide local, up-to-date news to the community. This is how you can continue to access our trusted content:
- Bookmark our website
- Make sure you are signed up for our breaking and regular headlines newsletters
- You can support us with a subscription
- Follow us on Twitter: @portmacnews
- Follow us on Instagram: @portmacnews
- Follow us on Google News


